An aging workforce. Unprecedented turnover. Increased absenteeism. The “Great Resignation” is turning the manufacturing industry upside down.
By 2030, the industry will be grappling with 2.1 million unfilled jobs, says a 2021 study from Deloitte, and nearly half of manufacturers say the worker shortage has led to missed revenue opportunities.
For the industry’s benefits teams and financial leaders, this presents an incredible challenge—but also an opportunity. Forward-thinking manufacturing companies are rethinking their benefits strategies to attract and retain the younger and more diverse workforce that they will need to succeed as an older generation of workers moves toward retirement. According to a recent report from CBIZ, “Organizations that choose to differentiate their benefits plans are likely to have an edge over those that stick with the status quo.”
Data analysis and predictive analytics can supercharge your benefit strategy, enabling you to select and evaluate health and wellness point solutions to determine which ones would have the biggest impact on your existing workforce and your workforce of the future.
Here are five data-backed strategies to improve the health, well-being, and productivity of your current and future employees:
1. Quantify the impact of new and existing programs on employee health, cost, retention, and productivity
For the younger generation, benefits and company culture matter – a lot. In four years, according to a Parsable study, millennials will comprise 75% of the workforce, and nearly half of millennials rank manufacturing as their second-to-last career choice.
According to the Connecticut Business & Industry Association, “The new generation of workers may not value longevity in a position more than other important factors, such as retention incentives, benefits, company culture, training, and an overall sense of value to the company.”
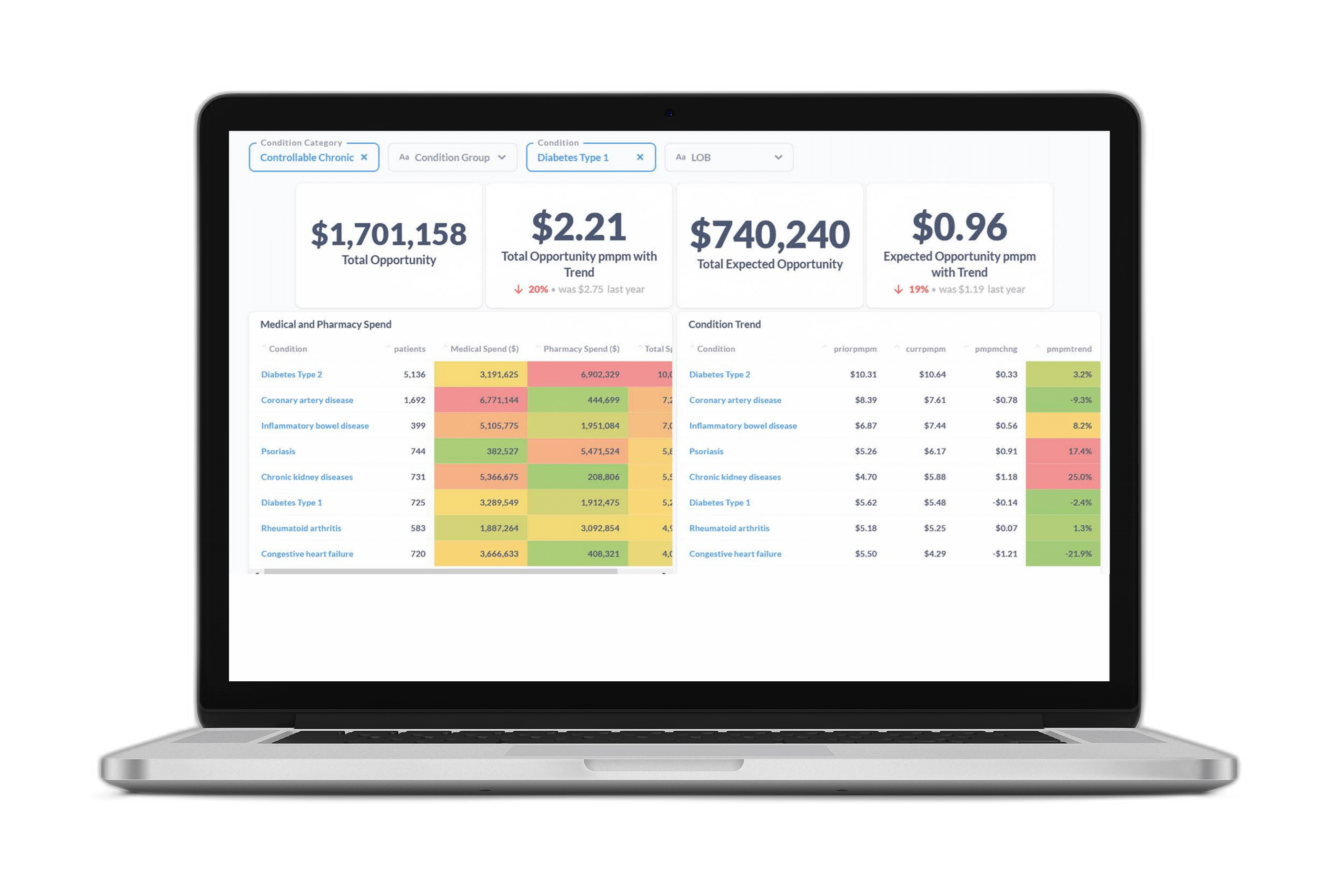
By leveraging predictive insights, manufacturing leaders like you can understand what benefit offerings will attract the right workers. An effective data partner will provide intuitive dashboards that tell you exactly what would and wouldn’t work to meet the unique needs of your existing employees and the ones you’re seeking to recruit.
With these insights, you’ll have the ability to proactively compare the impact of current and future benefit and wellness programs of health outcomes and cost. For instance, you’ll know the predicted ROI from different point solutions, such as disease management programs, fitness trackers, clinical outreach strategies, and more.
2. Align partners and vendors behind a value-based strategy
More manufacturing leaders are prioritizing diversity and inclusion initiatives in order to expand their traditionally male-dominated workforce and fill vacant jobs.
Benefits and wellness programs that attract and retain women, in particular, represent an opportunity to combat rising attrition and turnover rates. According to the Manufacturing Institute, women account for less than one-third of the manufacturing workforce despite representing nearly half of all workers.
As a result, more companies have begun offering health and wellness programs geared toward issues that affect women such as breast cancer and pregnancy risks.
As these new initiatives are implemented, it’s essential to have real-time updates on engagement and utilization rates to ensure they’re meeting the intended goals. Tracking the progress of these diversity-focused programs requires more than just traditional performance metrics. Your data and analytics solution should account for non-traditional data sources such as social determinants of health factors, including access to affordable housing, quality nutrition, and other non-clinical health barriers.
Armed with this intelligence, you will be able to share member-level risk profiles with health and vendor partners to set more accurate value-based goals and prioritize outreach efforts. These insights will also allow you and your partners to track performance guarantees in key areas such as diabetes management, musculoskeletal, behavioral health, weight loss, and smoking cessation.
3. Implement an effective strategy to reduce opioid dependence and improve mental health
The opioid epidemic and mental health issues have taken a significant toll on the manufacturing industry, affecting both productivity and contributing to the rising numbers of people leaving their jobs.
According to Industry Week, “In recent years, the opioid crisis has reached critical levels, and a new report by the MAPI Foundation shows an ominous geographic overlap between U.S. manufacturing-centric regions and opioid abuse.”
What if you could target those employees at risk for opioid dependence? What if you could pinpoint the areas of your workforce at risk for depression, or other existing and emerging mental health needs? And what if you knew how likely these employees would respond to certain types of outreach so that your efforts would make the biggest impact?
Predictive analytics give you this proactive insight, allowing you to design preventive mental health and wellness programs around opioid dependence and mental health issues that match the right employee to the right resource at the right time. That could mean anything from better educating members to existing wellness or therapeutic programs or expanding initiatives such as virtual care and telehealth.
4. Measure results to determine ROI
A major challenge for financial and benefit leaders in the manufacturing industry is a lack of hard numbers showing a program’s impact on health, productivity, and total cost of care. For many HR teams, benefits design is guesswork.
But forward-looking leaders know guesswork isn’t enough to build their workforce of the future. It’s important to be equipped with real-time updates on how programs are performing. An effective data partner will be able to integrate the wide array of success metrics and give you real, easy-to-understand numbers quantifying a solution’s impact.
This enables benefit and finance teams to transparently communicate their success to internal stakeholders, and successfully build business cases to expand existing programs or invest in new resources.
5. Continually refine your offerings to build a responsive benefits program for the future
There are an overwhelming number of point solutions for improving benefit design. How do you know which ones to choose? What will be most impactful to boost productivity, reduce costs, and retain high-quality talent, especially as the demands of a new generation of workers shift?
You invest a lot in your benefit and wellness programs. You shouldn’t have to wait for a year-end report to tell you that engagement is lacking, or that avoidable healthcare costs occurred because a specific population of workers needed, for example, mental health services rather than a diabetes prevention program.
Predictive insights give you the ability to evaluate current and future programs in real-time so you can be confident that you’re choosing the solutions that will help you fill jobs, retain workers, and reduce healthcare costs.
Want to learn more?
Certilytics is the transformative data and predictive analytics partner for a rapidly growing number of the nation’s largest healthcare organizations and employers that are leading the shift to AI-powered, value-focused decision-making.
Our Impact Evaluator helps employers maximize the impact of benefits programs by:
- Uncovering key opportunity areas to quantify the potential impact of new benefit and wellness programs
- Matching the right member to the right program at the right time to boost utilization and engagement
- Measuring program performance to demonstrate ROI
Check out our case study and see how we helped one Fortune 100 employer maximize benefits program impact and uncover $200PMPY in savings.