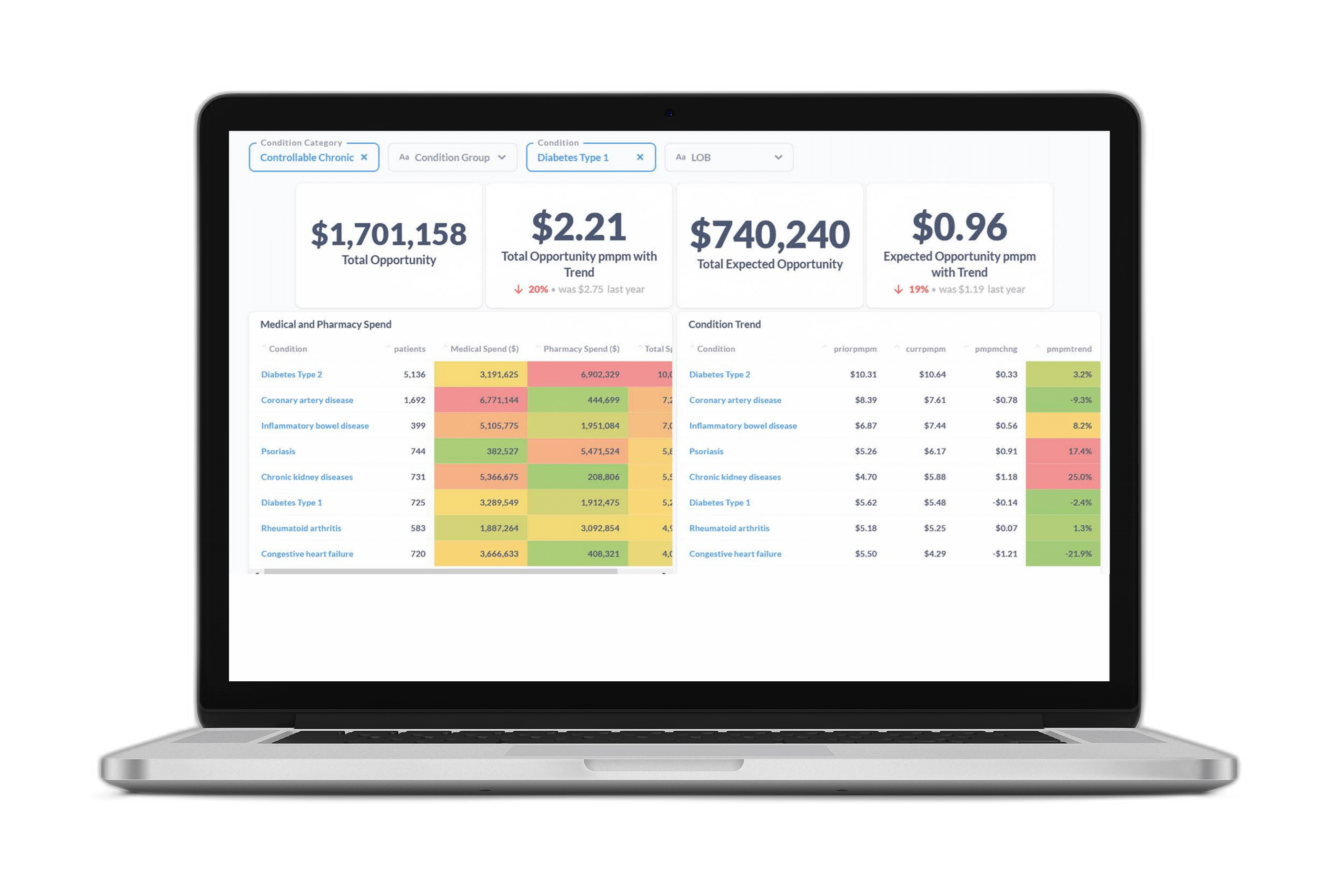
A big challenge for healthcare Data Science teams is building accurate predictive models at the member level when there’s a lack of historical data, typically during a member’s initial months of enrollment.
The Certilytics solution: integrating non-traditional data into our innovative approach to model development that leverages deep learning.
Augmented with non-traditional data, including provider treatment patterns, our model accuracy has improved significantly in limited-data settings—including our ability to identify members at risk of becoming High Cost Claimants (HCCs), defined as those whose annual costs exceed $100,000.
Because HCCs represent such an outsized—and growing—share of a population’s overall healthcare costs, there is considerable interest among payers in the early identification, or prediction, of members at risk of becoming HCCs. But this is especially difficult for new members who, by their very nature, have limited medical history—a major gap for care management teams.
Certilytics is able to overcome this challenge through the use of non-traditional data, building models that retain high accuracy even without access to lengthy member medical histories.
This solution represents millions of dollars in additional potential savings for our customers by way of significantly improved identification of HCCs during and following the first 90 days of new member enrollment.
You can also contact us to learn more about Certilytics’ product offerings, which leverage sophisticated data science and a highly scalable technology stack to put our customers at the forefront of machine learning in healthcare.