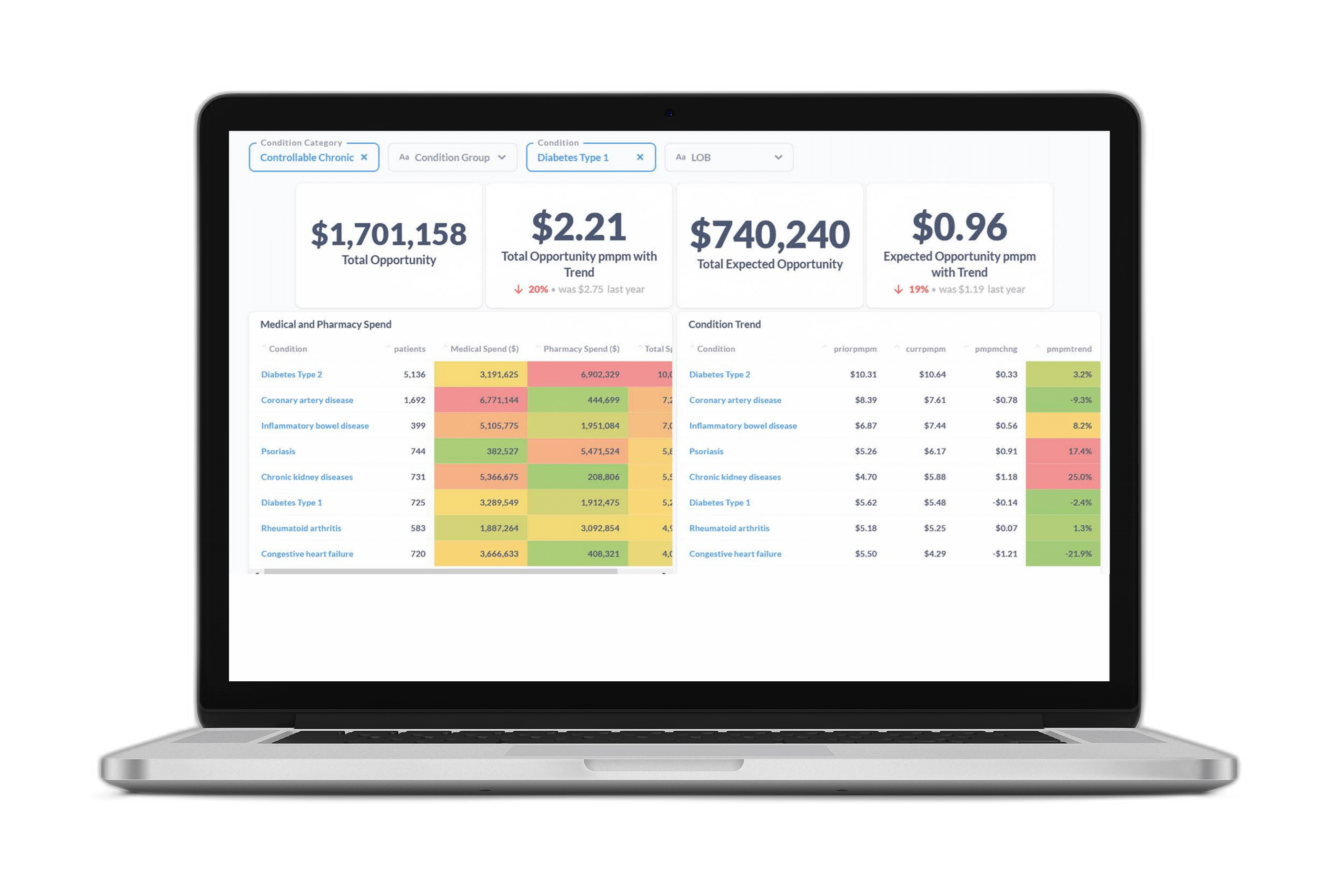
Now more than ever healthcare payers are looking for better ways to tackle heart disease and obesity and the rising healthcare costs associated with these conditions
Both are among the deadliest and costliest chronic diseases, driving up avoidable emergency room visits and exacerbating other conditions.
Obesity affects 20% of children and 42% of adults, putting them at risk for chronic diseases such as type 2 diabetes, heart disease, and some cancers. Cardiovascular disease is even deadlier, with more than 877,500 heart disease or stroke deaths in the U.S. each year, according to the CDC.
Combined, these two conditions cost the health system $389 billion annually.
How are payers starting to change this reality? Many are turning to predictive analytics to get more proactive before an avoidable health event occurs.
Here are the top three predictive models healthcare organizations should be using to improve heart health and prevent obesity:
1. Heart Disease Model
Every 40 seconds, someone in the United States has a heart attack, according to the CDC.
Predictive analytics has the ability to help detect those at risk for heart attacks before a catastrophic event occurs.
With this insight, payers can intervene earlier with the patients who need it most, including with strategies that help prevent the onset of other associated conditions.
2. Hospital Readmission Risk
Obesity increases the burden on hospitals by not only driving up the number of avoidable hospital visits but also lengthening the duration of hospital stays, studies have noted.
Predictive insights help healthcare organizations break the cycle of repeat hospital visits, helping pinpoint when obesity and heart disease are driving repeat visits.
Most of the time, payers are spending resources treating complications that stem from checking out a patient too early.
But armed with predictive insights, payers and providers are able to coordinate effective discharge planning from the time a patient checks into the hospital.
This ensures that the patient’s needs are met throughout the care continuum, helps reduce avoidable overspend, and addresses underlying causes for a hospital visit before a patient is readmitted.
3. SDoH Model
Payers can put preventive strategies in place, but if the targeted population doesn’t have adequate access to care, those resources may not be used to their full potential.
That’s why it’s important for payers to look at the impact of heart disease and obesity through a health equity lens.
With predictive models that focus on social determinants of health (SDoH), payers can pinpoint those segments of the population where resources and investments are needed most.
Effective SDoH predictive models also give healthcare leaders the ability to test hypotheses prior to implementing new programs to make sure they are creating real value.
That way, they know to prioritize outreach initiatives such as educational programs, placement of new clinics, or targeted telehealth outreach.
Did You Know?
- Certilytics’ “Hospital Readmission Risk” model leverages deep learning to predict a readmission within 30 days of discharge after an acute hospitalization.
- Certilytics’ “Heart Disease Model” calculates the risk that a member will suffer a heart attack within the next 12 months.
- Certilytics’ “SDoH Model” quantifies and predicts SDoH-derived risk. Our model answers not just the “who” and “where” of SDoH risk, but the “why” and “how.”
For a free consultation with our team of experts on how you can leverage predictive insights to transform your organization, reach out to us at contact@certilytics.com.